Hi everyone,
I can't believe how long it is since I last updated my blog, but the last 7 months has been a bit of a rollercoaster and has had several ups and many downs. It is not a period of time I ever wish to repeat but thankfully, despite how tough it's been, I have made it through and survived everything that has been thrown at me.
The big news, for anyone that hasn't heard, is that I am now in full remission from the Leukaemia and the tests I've had recently show that there are now signs of the disease even down to a molecular level. Thankfully all I have been through has been worthwhile.
When I last wrote I was about to embark on the transplant process, so in this blog update I'll spill the beans on everything that has happened since my readmission to hospital and how I've got to where I am today having beaten the disease, so this is going to be a lengthy post!
After I was admitted to the bone marrow unit on the 2nd January, I had a Hickman line fitted the following day, which made the administration of drugs and chemotherapy, and the taking of blood samples much simpler. It also got rid of the need to continually have cannulas inserted and was more reliable than the PICC line I'd had in my arm previously.
The first few days in hospital consisted of a progressively harsher course of chemotherapy drugs to effectively knock out my immune system and make room in my bone marrow for the new cells to be transplanted. Initially there were no ill effects from the treatment but things were about to get a lot tougher. This course of treatment also finished off my hair loss, and with the exception of my eyebrows, I now lost all of the hair on my body and head!
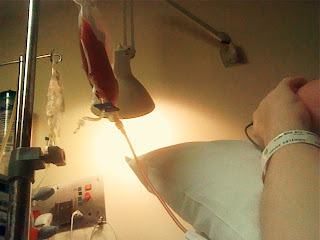
The transplant itself happened on the 10th January as planned and was more straightforward than I ever imagined. The cells came in the form of two bags, similar to those that had been used previously for blood transfusions and were delivered through the Hickman line over the course of about 3 hours late in the evening. By midnight it was all over and the new cells were circulating in my blood stream ready to find their way into my bone marrow and go to work. The photo below shows one of the bags of donor cells being transfused into me.
For the next couple of days I felt OK but soon after, the effect of the pre-transplant chemotherapy drugs kicked in with a vengeance. I was sick frequently and the contents of my bowels had the consistency of water! I ended up having to have a commode chair at the side of my bed as the frequent need to get to the toilet fast was overwhelming. I'll spare the gory details as I'm sure you can all probably imagine for yourselves.
The sickness and runny bum lasted for a couple of weeks and I became progressively weaker. Even standing long enough to be weighed on the scales in my room was difficult and I found myself feeling light headed if I stood for any longer than 30 seconds.
I've lost track of all the dates, but after the transplant I was probably in hospital for about 3-4 weeks, by which time my blood counts were starting to increase to a level that the medical team could think about letting me go home to continue my recovery.
I was discharged on a Friday evening and looking forward to going home to be with Andrea and the boys. My parents were also visiting that weekend. Unfortunately at the time I was starting to develop a fungal infection on my tongue which worsened over the weekend, making my mouth and my tongue in particular painfully sore.
I had a follow up appointment on the Monday and when they saw the state of my tongue, which was then white with the fungal infection, I was promptly readmitted to the room I'd left only a couple of days before.
This was probably the lowest point I'd been at throughout my treatment. When I was discharged before the weekend it had felt like I was making good progress after my transplant and things were on the up. Now, being brought back into hospital was a real blow and I felt like I'd taken a huge step backwards.
Over the next few days I was unable to eat due to the pain in my mouth and my tongue became even worse, with cracks and sores appearing all over it which made eating impossible and talking very difficult. Despite a rigorous routine of four different mouthwashes four times a day and anti-biotics, very little improvement was made against the infection and my weight dropped dramatically through a lack of nutrition.
The nursing staff became really worried about my demeanour as I appeared quite depressed to them, though I didn't realise it myself. Eventually they convinced me to let them refer me to a psychologist to discuss my feelings. A couple of days later the psychologist came to see me, by which time the pain in my mouth had started to ease and I was beginning to feel a little better. We had a good chat and I think she was satisfied by the end that I was indeed feeling better than I had.
A few days later I was discharged once again and resumed the slow process of recovering at home.
Much of my time was spent in bed as I was too weak to get up and make the journey downstairs, though occasionally I did manage and spent the day laid on the sofa, watching TV and sleeping. I survived at this time mainly on soups, tinned spaghetti and supplementary nutritional milk shakes. Slowly my appetite started to come back, as did my strength.
Hospital check ups consisted of a weekly visit to the bone marrow day unit for blood tests and a discussion with the consultant. Due to being so weak, Andrea had to drive me to hospital each week and drag me to the clinic in a wheelchair as I couldn't walk such a distance initially.
I did manage to regain enough strength after a few weeks and felt that I'd reached a big milestone when I was eventually strong enough to walk from the car park to the clinic, taking a couple of rests along the way.
Just as things were starting to improve I was struck with another blow when I picked up an influenza bug, which knocked my appetite once more and sapped my strength. Once more I wasn't eating and struggling to keep anything I did eat down. The strength I'd regained quickly vanished and my weight dropped dramatically.
This state seemed to last for weeks with no significant improvement. I got weaker all the time until things came to a head during one of my weekly visits to hospital. In the clinic the nurses had completed my observations, taking my blood pressure, checking my pulse, saturation levels and temperature. I was taken to be weighed, which involved sitting in a weighing chair. I remember the nurse starting to record my weight, then the next thing I remember I was laid on the floor surrounded by consultants and nursing staff with an oxygen mask being placed over my face. I'd collapsed in the chair and had been lowered to the floor by the nurses.
This now showed just how weak I'd become and unsurprisingly I was admitted to be kept overnight for observations. I spent the afternoon in the oncology assessment unit before being moved to the haematology ward where I'd spent much of my time during my treatment before Christmas. The following morning I was taken in a wheelchair by a porter for a chest x-ray. After the events of the previous day I warned the radiographer that I couldn't stand for long and sure enough after being stood in front of the chest stand for a few moments I started to feel light headed and had to sit down. Unfortunately the radiographer sat me sideways in a chair in front of the chest stand in the hope of still being able to get the x-ray.
With no support behind me, the next thing I remember was coming round, laid on the floor again with a very painful lump on the back of my head. I'd collapsed again and as I fell this time I hadn't had the luxury of being lowered to the floor and had crashed hard, banging the back of my head hard on the terrazzo floor of the x-ray room. Panic ensued as staff rushed to my aid and I was eventually helped back to my feet and onto a trolley where they finally managed to get the required x-ray.
As a consequence of my collapses, I ended up spending the whole week in the hospital, during which time I was also taken for an MRI scan of my head, and had a 24 hour ECG trace to record the performance of my heart. Neither showed any abnormalities so thankfully the reason for me collapsing wasn't down to my brain or my heart. The conclusion was reached that it was down to my general lack of strength which was a consequence of not eating properly and not getting any exercise.
Once again I returned home to continue my recovery but still struggled with my appetite and had difficulty keeping any nourishment down for any length of time.
Weeks passed and the weekly visits to the hospital continued, thankfully without any further episodes of collapsing. As time went on my skin also became very dry and flaky, particularly on my face. Despite this the results from my blood tests each week showed promising signs that the transplant was working and that the new cells were 'grafting' themselves into my system.
To counteract the dry skin I was applying a moisturiser to the affected areas but unwittingly, one day, I applied some to my face which it turned out, subsequently irritated my eyes. The following day I woke with a tremendous pain in my eyes and couldn't open them. When I eventually did manage to prise them open, my vision was severely blurred.
Fortunately I was due to attend hospital that day for my weekly visit. As Andrea drove me there it was a very bright sunny day, but due to the pain in my eyes I spent the journey with my eyes closed and a woolly hat pulled down over them to block out the brightness of the sun. We checked in to the bone marrow day unit where we told them about my eyes and they immediately made arrangements for me to go downstairs to the eye clinic and be seen straight away.
I was still unable to open my eyes until one of the nurses in the eye clinic dropped some local anaesthetic into my eyes. The pain subsided almost immediately and I was finally able to open my eyes but my vision was still very blurred. They examined my eyes and found that the surface was badly scratched in both eyes. I must have been rubbing them overnight due to the irritation after using the moisturiser. I was prescribed some ointments for my eyes and thankfully the following day my sight started to return and was back to normal within a couple of days.
Of all the senses, I can now imagine that losing your sight has to be possibly the worst. Not being able to see leaves you feeling totally helpless and dependant on others. For 24 hours at least I truly panicked, feeling that having defeated the Leukaemia I was now destined to go blind. Thankfully it wasn't the case but my heart really does go out to those that are unfortunate enough to lose their sight..
By now it was mid May, and as a result of my skin condition, the consultants decided I had a form of 'graft versus host disease' (GvHD) which is in effect my old cells fighting against the new ones. Consequently they prescribed a heavy dose of steroids to try and combat the GvHD. I have to say that the steroids are probably what really kick started my recovery and within a couple of days of starting the medication, my appetite began to return properly and I started to regain some strength.
Within a week of starting the steroids I managed to gain 4 Kg in weight and was able to start exercising more, though I was still very weak. I had a new found determination to regain my fitness and arranged the loan of a wheelchair from the British Red Cross. My theory was that I could go for short walks, pushing the wheelchair which would aid my balance, and that if I got tired I had a ready made seat to hand.
In the end my strength came back so rapidly that I only actually used the wheelchair a couple of times and within 2 weeks returned it to the Red Cross. Since then my strength has continued to progress and my appetite remains. As my skin condition slowly improved, the dose of steroids was reduced and I now remain on a low dosage. Thankfully my appetite has stayed and I am now eating more or less normally. My walks have increased in distance and now I don't have to give a second thought to walking anywhere whilst out, even to the degree that I walk every night with Andrea and the dog round our local country park. At the time though the transformation thanks to the steroids was unbelievably rapid and just the boost I needed.
Not long into my course of steroids I went to hospital for another bone marrow biopsy. This would show whether there was any sign of Leukaemia and give an indication of the proportion of new donor cells to my old ones. By now I was also able to drive myself to hospital after not driving for a period of some six months. It took a little while to get used to driving again, accompanied by Andrea, until I was confident enough to make the journey to hospital alone.
Within a couple of weeks the results of the biopsy came back and on the 22nd May I got confirmation that I was in remission with no sign of the Leukaemia. Further good news came on the 5th June when I was told that my bone marrow was now 100% donor.
My treatment continues in the form of daily medication, largely anti-rejection drugs and immuno-suppressants, together with a low dose of steroids. Every 3 months for the next two years I have to have a lumbar puncture and have chemotherapy injected into my spine to make sure my central nervous system stays clear.
Following a consultation last week at Nottingham City Hospital, I am also about to commence a course of treatment called Extracorporeal Photophoresis (ECP). This involves being connected to a machine for three hours per day, two days per week, every two weeks, initially for sixteen weeks. The machine takes blood from a vein in one arm, separates the white and red cells, mixes the white cells with a UV sensitive chemical and exposes them to UV light. The red and white cells are then returned to me via a vein in the other arm. The theory is that this treatment kills off the bad white cells that are causing my GvHD and over the course of the treatment my body recognises what is going on and attacks the remaining bad cells. This should hopefully resolve my GvHD and my skin conditions should improve.
In the meantime I have been making moves towards easing back into working life. Due to my on-going treatment and immuno-suppression, there are restrictions on what I can currently do and these mean that at the moment I am unable to return fully to work, particularly on a live construction site as I had been prior to my illness. I am therefore hoping to work from home and assist with some of the bids to win new work.
Slowly but surely I finally feel like my life is returning to normal and whilst I will continue to be under the control of the medical team for some time (and no doubt remain so for the rest of my life), the frequency of my check ups will reduce, as will the medication I'm on, allowing me to return to as normal a life as it can be.
With my health improved my thoughts are now turning back to my plans to walk up Snowdon in aid of Leukaemia and Lymphoma Research. Over the next couple of weeks I'll be approaching those that have previously shown an interest in joining me, and anyone else who's interested in tagging along with a view to finalising arrangements for the walk. My target is to complete it by the end of September, which would take me to just over a year from first being diagnosed. if you want to join me on the walk, please let me know.
I'll write again as plans come together for the walk, but for now, thanks for reading.
Steve.
Dieseldrinkers Road To Recovery
The story of my fight against Acute Lymphoblastic Leukaemia (ALL).
Wednesday, 31 July 2013
Tuesday, 8 January 2013
A rough end to 2012
Hi everybody,
I've been conscious of the need to update you all via the blog for some time, but to be honest the end of 2012 was particularly tough and tiring, so the energy and motivation to write the blog has been very low.
The Methatrexate treatment that I had before Christmas was particularly draining and I had barely recovered fully from the first session before I was hit with the second dose and it effectively knocked the stuffing out of me.
I was discharged just before Christmas, so did spend it at home with Andrea and the boys, though with the exception of a few hours on Christmas day and New Years Eve, the holiday was spent in bed feeling very tired.
The New Year has started with me being re-admitted to hospital on the 2nd, but hopefully on the final leg of my journey as I am now recieving final preparatory chemotherapy before receiving new stem cells from a donor in a couple of days on the 10th January. My transplant is therefore finally happening.
My fingers are then crossed for a successful graft without complications, though even then the full recovery is likely to take another 6 months before life can get back to anywhere near normal.
Updates are likely to be few and far between and will be brief when I can, but please cross your fingers for me that things go smoothly.
All the best and thanks for reading.
I've been conscious of the need to update you all via the blog for some time, but to be honest the end of 2012 was particularly tough and tiring, so the energy and motivation to write the blog has been very low.
The Methatrexate treatment that I had before Christmas was particularly draining and I had barely recovered fully from the first session before I was hit with the second dose and it effectively knocked the stuffing out of me.
I was discharged just before Christmas, so did spend it at home with Andrea and the boys, though with the exception of a few hours on Christmas day and New Years Eve, the holiday was spent in bed feeling very tired.
The New Year has started with me being re-admitted to hospital on the 2nd, but hopefully on the final leg of my journey as I am now recieving final preparatory chemotherapy before receiving new stem cells from a donor in a couple of days on the 10th January. My transplant is therefore finally happening.
My fingers are then crossed for a successful graft without complications, though even then the full recovery is likely to take another 6 months before life can get back to anywhere near normal.
Updates are likely to be few and far between and will be brief when I can, but please cross your fingers for me that things go smoothly.
All the best and thanks for reading.
Friday, 23 November 2012
The next stage.
Hi everyone.
I've been at home since my last blog so there hasn't been much to update until now, but after yesterdays visit to the hospital for a blood test and meeting with the consultant I know what the immediate future holds as far as treatment is concerned. I also have news regarding the possible conclusion to my journey.
Since leaving hospital last Tuesday I've been back for blood tests last Thursday and this Tuesday and Thursday. Each time I've been given an update on my blood counts which have been steadily improving. As mentioned yesterday's visit also consisted of a longer discussion with the consultant which confirmed that my white cells, particularly my Neutrophils, (which are the white cells which fight infection) have improved to a level which are at the lower level of normal.
My red cell counts are not growing as quickly and I'm a little anaemic at the moment, but the counts are improving nevertheless. Being anaemic means doing anything which requires exertion saps my energy quickly and I seem to feel this most in my legs. Climbing stairs or walking even a short distance soon has me out of breath and my head pounding as my weak blood pumps around my body. Whilst I'm in hospital the normal solution is a transfusion and when I return it is still a possibility, even though my own system is coming back to life.
So my bone marrow is slowly recovering which is good news, though it has taken quite some time.
The induction phase of my treatment is therefore over and as the consultant said yesterday its usually easy to get patients into remission during this stage, as they have with me. The trick is keeping them there and making sure that the Leukaemia doesn't come back.
The next phase of the treatment was therefore explained to me yesterday and I was presented with a new plan for the next 28 days of treatment. Fortunately the treatment doesn't start until next Monday so I do at least have the weekend at home.
So when I return on Monday, subject to satisfactory results from blood and urine tests I will be put on a drip to hydrate me, which is to reduce the risk of damage to my liver. After this I will be given Methatrexate, which is the chemotherapy drug that I have previously had injected into my spine. This time it will be delivered intravenously over a long period. By all accounts the possible side effects are a sore mouth, sickness and diarrhoea, so I'm hoping I don't suffer too much.
At the end of the delivery of the Methatrexate, which I seem to remember is a 24 hour period, a form of folic acid is given to counteract the effects and help settle things down.
The other procedure that was planned for Monday was the installation of a new PICC line in my arm to make administration of drugs and taking blood sample easier. I'd had one installed previously but due to an infection on the skin surrounding the entry site it was taken out about a week after installation. This was probably due to my low neutrophil count at the time. However I got a surprise call from the hospital this morning to say that the list for Monday was full but that they'd had a cancellation on the list for this afternoon and could I make it to have my line installed today. Fortunately I could, so I've been this afternoon ad now have a fresh line in my arm ready for Monday.
The indications are that if treatment is started on Monday, by Thursday I should be well enough to go home again. I'll then have a full week off without treatment and on day 15 the process with the Methatrexate and folic acid is repeated.
In effect that's it for this next phase of treatment which doesn't sound much but could potentially have two short periods of discomfort and illness after each administration of Methatrexate. All being well it will also be over in time for Christmas so that I can have a break to celebrate with my family over the holiday period.
The consultant also gave me some good news yesterday by indicating that a donor has been located for a bone marrow transplant, which will give me the best chance of cure and survival. The likelihood is that the transplant process will start early in the new year and will probably mean an extended stay (probably 2-3 months) in hospital following transplant whilst the graft hopefully occurs and my system starts to recover. I'll know more about the full process when the time gets nearer.
I'll report next week on how the treatment is progressing (providing I feel up to it).
Finally I want to give a mention to a brave (possibly mad) lady that is taking part in a gruelling 8 mile cross country run over land normally used to test army vehicles. The event is suitably titled 'The Grim Challenge' and takes place in a couple of weeks time at the beginning of December near Aldershot.
Nicole Baynton is the lady in question and is a good friend I have made through my association with Towcestrians Rugby Club, where our sons play rugby together. She contacted me whilst I was in hospital recently to ask whether she could help raise funds for my preferred charity, Leukaemia and Lymphoma Research. I'm delighted to say she has my full support and send my best wishes with her for successfully completing the run. I'll have a Guinness or two with her down at the Tows club sometime in the future to celebrate.
Nicole has a JustGiving page, so my plea is for anyone that can to join me in my support of her on this run, for which I'd be very grateful. Nicole's page can be found here (http://www.justgiving.com/Nicole-Lisa-Helen).
All the best to everybody and thanks for reading.
I've been at home since my last blog so there hasn't been much to update until now, but after yesterdays visit to the hospital for a blood test and meeting with the consultant I know what the immediate future holds as far as treatment is concerned. I also have news regarding the possible conclusion to my journey.
Since leaving hospital last Tuesday I've been back for blood tests last Thursday and this Tuesday and Thursday. Each time I've been given an update on my blood counts which have been steadily improving. As mentioned yesterday's visit also consisted of a longer discussion with the consultant which confirmed that my white cells, particularly my Neutrophils, (which are the white cells which fight infection) have improved to a level which are at the lower level of normal.
My red cell counts are not growing as quickly and I'm a little anaemic at the moment, but the counts are improving nevertheless. Being anaemic means doing anything which requires exertion saps my energy quickly and I seem to feel this most in my legs. Climbing stairs or walking even a short distance soon has me out of breath and my head pounding as my weak blood pumps around my body. Whilst I'm in hospital the normal solution is a transfusion and when I return it is still a possibility, even though my own system is coming back to life.
So my bone marrow is slowly recovering which is good news, though it has taken quite some time.
The induction phase of my treatment is therefore over and as the consultant said yesterday its usually easy to get patients into remission during this stage, as they have with me. The trick is keeping them there and making sure that the Leukaemia doesn't come back.
The next phase of the treatment was therefore explained to me yesterday and I was presented with a new plan for the next 28 days of treatment. Fortunately the treatment doesn't start until next Monday so I do at least have the weekend at home.
So when I return on Monday, subject to satisfactory results from blood and urine tests I will be put on a drip to hydrate me, which is to reduce the risk of damage to my liver. After this I will be given Methatrexate, which is the chemotherapy drug that I have previously had injected into my spine. This time it will be delivered intravenously over a long period. By all accounts the possible side effects are a sore mouth, sickness and diarrhoea, so I'm hoping I don't suffer too much.
At the end of the delivery of the Methatrexate, which I seem to remember is a 24 hour period, a form of folic acid is given to counteract the effects and help settle things down.
The other procedure that was planned for Monday was the installation of a new PICC line in my arm to make administration of drugs and taking blood sample easier. I'd had one installed previously but due to an infection on the skin surrounding the entry site it was taken out about a week after installation. This was probably due to my low neutrophil count at the time. However I got a surprise call from the hospital this morning to say that the list for Monday was full but that they'd had a cancellation on the list for this afternoon and could I make it to have my line installed today. Fortunately I could, so I've been this afternoon ad now have a fresh line in my arm ready for Monday.
The indications are that if treatment is started on Monday, by Thursday I should be well enough to go home again. I'll then have a full week off without treatment and on day 15 the process with the Methatrexate and folic acid is repeated.
In effect that's it for this next phase of treatment which doesn't sound much but could potentially have two short periods of discomfort and illness after each administration of Methatrexate. All being well it will also be over in time for Christmas so that I can have a break to celebrate with my family over the holiday period.
The consultant also gave me some good news yesterday by indicating that a donor has been located for a bone marrow transplant, which will give me the best chance of cure and survival. The likelihood is that the transplant process will start early in the new year and will probably mean an extended stay (probably 2-3 months) in hospital following transplant whilst the graft hopefully occurs and my system starts to recover. I'll know more about the full process when the time gets nearer.
I'll report next week on how the treatment is progressing (providing I feel up to it).
Finally I want to give a mention to a brave (possibly mad) lady that is taking part in a gruelling 8 mile cross country run over land normally used to test army vehicles. The event is suitably titled 'The Grim Challenge' and takes place in a couple of weeks time at the beginning of December near Aldershot.
Nicole Baynton is the lady in question and is a good friend I have made through my association with Towcestrians Rugby Club, where our sons play rugby together. She contacted me whilst I was in hospital recently to ask whether she could help raise funds for my preferred charity, Leukaemia and Lymphoma Research. I'm delighted to say she has my full support and send my best wishes with her for successfully completing the run. I'll have a Guinness or two with her down at the Tows club sometime in the future to celebrate.
Nicole has a JustGiving page, so my plea is for anyone that can to join me in my support of her on this run, for which I'd be very grateful. Nicole's page can be found here (http://www.justgiving.com/Nicole-Lisa-Helen).
All the best to everybody and thanks for reading.
Wednesday, 14 November 2012
Home again.
Afternoon all.
I'll start with some good news and can report that as of last night I was allowed home for a few days after my blood counts had recovered sufficiently to reduce my risk of infection. They are still very low though so whilst I'm home I need to be sensible and take care in everything I do.
At this stage I don't know how long this respite will last and it is dependant on the next stage of treatment, more of which will be revealed tomorrow when I return to the hospital for a blood test and meeting with the consultants.
From the discussions I've had so far it looks like there are two options for the next stage. The first is to have a weekly treatment of Methatrexate, which is what I've been having injected into my spine. This time it will be injected intravenously to keep the protection up against the return of the leukaemia until such time as a bone marrow donor can be found.
The second option is to go directly into transplant and the hospital were hoping for some news over a possible match from the bone marrow registry before I return on Thursday.
Personally I'm hoping that transplant can be held off until after Christmas as it will be a long recovery period afterwards and I really don't want to be in hospital over Christmas.
Either way it's likely that I won't restart treatment until a week on Monday since my body needs adequate time for my bone marrow to recover and my blood counts to grow to an acceptable level before it gets knocked back again. This should give me a reasonable break to spend at home with my family.
Since my last blog I've had two more blood transfusions and two more units of platelets. This brings my total to 15 units of blood and about 5 of platelets. To anyone that is a blood donor, many thanks. During treatment like I'm going through and my fellow patients, donated blood is vital in ensuring that we can survive whilst our own blood manufacturing systems are not functioning.
Transfusion of platelets has previously been uneventful but the middle of last week I had a unit which brought me out in a severe rash, almost like a nettle rash all over my body, which was agonisingly itchy and was only brought under control by the administration of some intravenous Piriton. I still had to put up with the itching for a painful couple of hours until the rash finally subsided. Since then I've had another unit of platelets which was preceded with a precautionary dose of Piriton.
I've also previously had a mild reaction during a transfusion of blood, but last Friday I had a much more severe reaction. This started out about 6pm as strong shivering which lasted about two hours in total. The blood transfusion was stopped about half an hour after the shivering started and again I needed to be given Piriton to deal with the allergic reaction. This could only be done after my cannula had been replaced as the one used for the blood had started to leak. About half to three quarters of an hour after the Piriton was given the shivering finally stopped, but my then temperature shot up to 38.7 degrees and I was burning up. I was given Paracetemol at about 10pm to deal with my temperature and by 1am the next morning thankfully things had settled down and were back to normal.
I had my final unit of blood and a unit of platelets yesterday before being discharged, both preceded with a dose of Piriton. A blood test that was taken about an hour after the transfusions had finished should give the medical staff an indication as to whether I'm developing a resistance to transfusion, since these adverse reactions seem to be worsening.
I should know more about my treatment so far and the next steps after seeing the consultants tomorrow and will update you all via my next blog.
For the time being though I'll be making the most of my time at home. There are a few jobs that need doing in the garden and in my frail state it's time for my boys to step up and do some work, supervised by me, to get the garden ready for winter. So, though they don't know it yet, I have a weekends gardening planned for them!
Thats all for now so as always, thanks for reading.
I'll start with some good news and can report that as of last night I was allowed home for a few days after my blood counts had recovered sufficiently to reduce my risk of infection. They are still very low though so whilst I'm home I need to be sensible and take care in everything I do.
At this stage I don't know how long this respite will last and it is dependant on the next stage of treatment, more of which will be revealed tomorrow when I return to the hospital for a blood test and meeting with the consultants.
From the discussions I've had so far it looks like there are two options for the next stage. The first is to have a weekly treatment of Methatrexate, which is what I've been having injected into my spine. This time it will be injected intravenously to keep the protection up against the return of the leukaemia until such time as a bone marrow donor can be found.
The second option is to go directly into transplant and the hospital were hoping for some news over a possible match from the bone marrow registry before I return on Thursday.
Personally I'm hoping that transplant can be held off until after Christmas as it will be a long recovery period afterwards and I really don't want to be in hospital over Christmas.
Either way it's likely that I won't restart treatment until a week on Monday since my body needs adequate time for my bone marrow to recover and my blood counts to grow to an acceptable level before it gets knocked back again. This should give me a reasonable break to spend at home with my family.
Since my last blog I've had two more blood transfusions and two more units of platelets. This brings my total to 15 units of blood and about 5 of platelets. To anyone that is a blood donor, many thanks. During treatment like I'm going through and my fellow patients, donated blood is vital in ensuring that we can survive whilst our own blood manufacturing systems are not functioning.
Transfusion of platelets has previously been uneventful but the middle of last week I had a unit which brought me out in a severe rash, almost like a nettle rash all over my body, which was agonisingly itchy and was only brought under control by the administration of some intravenous Piriton. I still had to put up with the itching for a painful couple of hours until the rash finally subsided. Since then I've had another unit of platelets which was preceded with a precautionary dose of Piriton.
I've also previously had a mild reaction during a transfusion of blood, but last Friday I had a much more severe reaction. This started out about 6pm as strong shivering which lasted about two hours in total. The blood transfusion was stopped about half an hour after the shivering started and again I needed to be given Piriton to deal with the allergic reaction. This could only be done after my cannula had been replaced as the one used for the blood had started to leak. About half to three quarters of an hour after the Piriton was given the shivering finally stopped, but my then temperature shot up to 38.7 degrees and I was burning up. I was given Paracetemol at about 10pm to deal with my temperature and by 1am the next morning thankfully things had settled down and were back to normal.
I had my final unit of blood and a unit of platelets yesterday before being discharged, both preceded with a dose of Piriton. A blood test that was taken about an hour after the transfusions had finished should give the medical staff an indication as to whether I'm developing a resistance to transfusion, since these adverse reactions seem to be worsening.
I should know more about my treatment so far and the next steps after seeing the consultants tomorrow and will update you all via my next blog.
For the time being though I'll be making the most of my time at home. There are a few jobs that need doing in the garden and in my frail state it's time for my boys to step up and do some work, supervised by me, to get the garden ready for winter. So, though they don't know it yet, I have a weekends gardening planned for them!
Thats all for now so as always, thanks for reading.
Thursday, 1 November 2012
I'm still in hospital.
Afternoon all.
As expected at the end of last week, I'm still in hospital due to my neutrophil count being low. In fact my count on Tuesday, when I hoped to go home for the boys birthday was 0.00 - absolute zero meaning my immune system was non existent. In addition to that my temperature has 'spiked' a couple of times over the weekend and increased for short periods up to at the most 37.8 degrees, which is an indication of a potential infection.
On Monday evening I was told that a bed had become available in the Bone Marrow Transplant unit, where I spent the early days of my treatment, and I was moved back down there about 8pm. Its good to have more space and a room of my own with the en-suite and widescreen TV, but I do miss the company of the patients around me. Since arriving on Monday I have been told that because my count is so low I am confined to my room since its filtered, positive pressure ventilation will reduce the risk of me being infected from the less sterile areas outside my room.
All of this unfortunately meant that much to my disappointment, I wasn't able to go home for the day and spend some time at home with the boys and Andrea. They did come in to the hospital mid morning and spent a couple of hours here. They brought their birthday cards and presents with them and opened them in my hospital room. I suppose there is an advantage to being back in the bone marrow unit in that at least we can have some private time together as a family, which the flimsy curtains around a bedded bay did not afford.
The boys both got a mobile phone each which they've been nattering about for years. Andrea finally gave in, but at least its gives us some comfort that they can keep in touch remotely whilst they are out - as long as they dont lose them! They also got a variety of presents and lots of money, cheques and vouchers so I've no doubt they'll be planning what to spend that on in no time.
My treatment for this phase has now finished completely. The last intra-veinous chemotherapy was given on Monday and I completed the chemotherapy tablets yesterday. So now my bone marrow has a chance to recover its function and already my neutrophil count is growing - up to 0.1 yesterday.
I'm on anti-biotics at the moment to rid my body of the infection that has generated the temperature spikes, and was detected in my blood samples. This also appears to be working such that my temperature has been more consistent today and my headache that has been almost constant for the past month is also easing.
My appetite has been waning a little over the past few days but the dietitian has been to see me today and indicated that as I'm managing to generally maintain my weight, there is no undue cause for alarm.
The doctors visit this morning indicated that I'm more or less certain to spend the weekend here but that as long as my counts continue to increase satisfactorily and my body responds to the anti-biotics there is some potential that I might be allowed home sometime next week for a period of recuperation.
I've been prescribed another two units of blood, which will take my total to ten, and expect to receive these either later today or tomorrow. These usually give me a boost of energy for a short period but hopefully as my bone marrow recovers it will pick up the production of my own blood and I won't need too many other transfusions for the time being at least.
I live in hope then and will tolerate my period of solitary confinement as best I can, as I know that reducing my exposure to the risk of infection will hopefully speed up my recovery and the chances of getting home for a break.
On Monday I managed to spend some time editing my book to incoroprate the changes I picked up during my proof reading, and got about half way through. I hope to use my remaining time in the bone marrow unit to complete this exercise and hopefully take the book to the next stage towards publishing.
Thanks again for reading.
As expected at the end of last week, I'm still in hospital due to my neutrophil count being low. In fact my count on Tuesday, when I hoped to go home for the boys birthday was 0.00 - absolute zero meaning my immune system was non existent. In addition to that my temperature has 'spiked' a couple of times over the weekend and increased for short periods up to at the most 37.8 degrees, which is an indication of a potential infection.
On Monday evening I was told that a bed had become available in the Bone Marrow Transplant unit, where I spent the early days of my treatment, and I was moved back down there about 8pm. Its good to have more space and a room of my own with the en-suite and widescreen TV, but I do miss the company of the patients around me. Since arriving on Monday I have been told that because my count is so low I am confined to my room since its filtered, positive pressure ventilation will reduce the risk of me being infected from the less sterile areas outside my room.
All of this unfortunately meant that much to my disappointment, I wasn't able to go home for the day and spend some time at home with the boys and Andrea. They did come in to the hospital mid morning and spent a couple of hours here. They brought their birthday cards and presents with them and opened them in my hospital room. I suppose there is an advantage to being back in the bone marrow unit in that at least we can have some private time together as a family, which the flimsy curtains around a bedded bay did not afford.
The boys both got a mobile phone each which they've been nattering about for years. Andrea finally gave in, but at least its gives us some comfort that they can keep in touch remotely whilst they are out - as long as they dont lose them! They also got a variety of presents and lots of money, cheques and vouchers so I've no doubt they'll be planning what to spend that on in no time.
My treatment for this phase has now finished completely. The last intra-veinous chemotherapy was given on Monday and I completed the chemotherapy tablets yesterday. So now my bone marrow has a chance to recover its function and already my neutrophil count is growing - up to 0.1 yesterday.
I'm on anti-biotics at the moment to rid my body of the infection that has generated the temperature spikes, and was detected in my blood samples. This also appears to be working such that my temperature has been more consistent today and my headache that has been almost constant for the past month is also easing.
My appetite has been waning a little over the past few days but the dietitian has been to see me today and indicated that as I'm managing to generally maintain my weight, there is no undue cause for alarm.
The doctors visit this morning indicated that I'm more or less certain to spend the weekend here but that as long as my counts continue to increase satisfactorily and my body responds to the anti-biotics there is some potential that I might be allowed home sometime next week for a period of recuperation.
I've been prescribed another two units of blood, which will take my total to ten, and expect to receive these either later today or tomorrow. These usually give me a boost of energy for a short period but hopefully as my bone marrow recovers it will pick up the production of my own blood and I won't need too many other transfusions for the time being at least.
I live in hope then and will tolerate my period of solitary confinement as best I can, as I know that reducing my exposure to the risk of infection will hopefully speed up my recovery and the chances of getting home for a break.
On Monday I managed to spend some time editing my book to incoroprate the changes I picked up during my proof reading, and got about half way through. I hope to use my remaining time in the bone marrow unit to complete this exercise and hopefully take the book to the next stage towards publishing.
Thanks again for reading.
Friday, 26 October 2012
Good news and bad news.
Afternoon all.
Just a quick update with a mixture of good news and bad news.
In the time honoured traditon I'll give the good news first, which doesn't actually concern me, but is an update on the patient that was in the bed next to me previouslay and who as you'll know from my blogs was quite ill. He was also the inspiration that really boosted my determination to raise funds for Leukaemia and Lymphoma research.
A couple of days ago I had an email from him. He's been at home since being discharged after the last time I was him when he was looking much better. His email was to let me know he'd had the result of a scan to check on the result of his treatment which had shown that his results were good and that the chemo had worked, leaving him clear which is great news. He doesn't require further treatment and has another scan in January to check that he is still clear so I wish him all the best.
Now to the bad news which relates to my ability to go home after this course of treatment which was my hope. During the consultants rounds early yesterday I was told that unfortunately due to my blood counts being so low at the moment my immune system is at absolute rock bottom, the lowest it has ever been. This means that before I can even be considered to be allowed home my system has to recover adequately to give my body a chance against infection which is likely to take at least a couple of weeks.
This wasn't what I wanted to hear but unfortunately it's something I have to resign myself to as I cannot afford to risk picking up an infection and becoming ill as a result. A prolonged stay in hospital will mean that any infection I pick up can be treated immediately and continuous monitoring of my temperature and condition will quickly identify any problems.
I had my final lumbar puncture of this phase yesterday and spoke to one of the other consultants who has been treating me. He recognised that am showing signs of 'cabin fever' as he called it and to his credit is hoping that a days home leave can be arranged so that I can at least go home for the boys birthdays on Tuesday. I really do have to avoid any risks over the weekend and make sure I maintain my fitness to have any hope of spending the day with them on their birthday.
As disappointing as it is to face the reality of what is likely to be another two or three weeks in hospital, the glimmer of hope of being able to spend the day with the boys and Andrea on their bitrhday will hopefully make it more special for them and is something I'll try hard to make happen if I can.
As far as treatment is concerned I've had a couple of days without treatment up to my lumbar puncture yesterday, which again went without a hitch. I woke with a headache this morning but I think that was more a result or a rough nights sleep than the spinal intervention.
This morning after encountering increased difficulties finding locations for the doctors to insert cannula's, I've been for a PICC (Peripherally Inserted Central Catheter) line fitting. This is in effect a tube that has been inserted into a vein high in my left arm and passes through my veins into my chest close to my heart. This allows any intra-veinous treatment to be injected through the PICC line, and for blood samples to be taken from it. The line should last for up to a year and will save the need to continually have needles poked into me for various reasons.
The line was inserted under a local anaesthetic after first establishing the location of a good sized vein using ultrasound. I had expected to feel the 45cm tube being fed into my veins but other than the initial needle for the anaesthetic I didn't feel a thing, and was surprised when the x-ray to check the final location of the tube came up on the screen and it was already in position.
So hopefully this line will see me through the remainder of my treatment without me having to be jabbed by too many more needles, other than those for lumbar puncture and bone marrow biopsies which unfortunately can't be avoided.
Thanks for reading.
Just a quick update with a mixture of good news and bad news.
In the time honoured traditon I'll give the good news first, which doesn't actually concern me, but is an update on the patient that was in the bed next to me previouslay and who as you'll know from my blogs was quite ill. He was also the inspiration that really boosted my determination to raise funds for Leukaemia and Lymphoma research.
A couple of days ago I had an email from him. He's been at home since being discharged after the last time I was him when he was looking much better. His email was to let me know he'd had the result of a scan to check on the result of his treatment which had shown that his results were good and that the chemo had worked, leaving him clear which is great news. He doesn't require further treatment and has another scan in January to check that he is still clear so I wish him all the best.
Now to the bad news which relates to my ability to go home after this course of treatment which was my hope. During the consultants rounds early yesterday I was told that unfortunately due to my blood counts being so low at the moment my immune system is at absolute rock bottom, the lowest it has ever been. This means that before I can even be considered to be allowed home my system has to recover adequately to give my body a chance against infection which is likely to take at least a couple of weeks.
This wasn't what I wanted to hear but unfortunately it's something I have to resign myself to as I cannot afford to risk picking up an infection and becoming ill as a result. A prolonged stay in hospital will mean that any infection I pick up can be treated immediately and continuous monitoring of my temperature and condition will quickly identify any problems.
I had my final lumbar puncture of this phase yesterday and spoke to one of the other consultants who has been treating me. He recognised that am showing signs of 'cabin fever' as he called it and to his credit is hoping that a days home leave can be arranged so that I can at least go home for the boys birthdays on Tuesday. I really do have to avoid any risks over the weekend and make sure I maintain my fitness to have any hope of spending the day with them on their birthday.
As disappointing as it is to face the reality of what is likely to be another two or three weeks in hospital, the glimmer of hope of being able to spend the day with the boys and Andrea on their bitrhday will hopefully make it more special for them and is something I'll try hard to make happen if I can.
As far as treatment is concerned I've had a couple of days without treatment up to my lumbar puncture yesterday, which again went without a hitch. I woke with a headache this morning but I think that was more a result or a rough nights sleep than the spinal intervention.
This morning after encountering increased difficulties finding locations for the doctors to insert cannula's, I've been for a PICC (Peripherally Inserted Central Catheter) line fitting. This is in effect a tube that has been inserted into a vein high in my left arm and passes through my veins into my chest close to my heart. This allows any intra-veinous treatment to be injected through the PICC line, and for blood samples to be taken from it. The line should last for up to a year and will save the need to continually have needles poked into me for various reasons.
The line was inserted under a local anaesthetic after first establishing the location of a good sized vein using ultrasound. I had expected to feel the 45cm tube being fed into my veins but other than the initial needle for the anaesthetic I didn't feel a thing, and was surprised when the x-ray to check the final location of the tube came up on the screen and it was already in position.
So hopefully this line will see me through the remainder of my treatment without me having to be jabbed by too many more needles, other than those for lumbar puncture and bone marrow biopsies which unfortunately can't be avoided.
Thanks for reading.
Wednesday, 24 October 2012
I'm OK everybody.
Hi all,
I know some of you are concerned about me as I haven't updated the blog for a week so I thought I ought to give you a brief update to let you know I'm still OK.
There is no doubt that this phase of treatment has hit me much harder than the previous phase and it has certainly knocked the stuffing out of me. It has left me feeling tired most of the time, nauseous and sick some of the time, and for the past three weeks I've had almost a constant headache. Consequently most of my days have been spent drifting in and out of sleep due to feeling exhausted and to help pass the days avoiding the pain or sickness I have felt at times.
My energy levels are low anyway as the chemotherapy is designed to inhibit the overall function of my bone marrow as well as attacking the cancerous cells within it. This not only slows down the production of my white cells which have been affected by the Leukaemia but also slows down the red haemaglobin cells which are vital for carrying the oxygen around my body, and the production of platelets which help my blood to clot. As a consequence during this stay in hospital, which has been two and a half weeks so far, I have had three blood transfusions (six units of blood in total), and two transfusions of a unit of platelets. I'm also due to have another unit of platelets before my final lumbar puncture tomorrow.
The stay in hospital is becoming monotonous and tiresome and on many occasions I find the highlight of a morning or afternoon is when the meal trolleys come around and I get something to eat - when I've felt up to eating that is. In between those times I've plugged in my headphones and laid back on my bed listening to music, trying to shut out the sound of what is going on around me which helps me to sleep. At times I've actually slept through the morning or afternoon snack rounds and missed out on a drink of tea, or hot chocolate, and have sometimes found the nurses struggling to wake me from a deep slumber in order to check my blood pressure and temperature when they do the obs rounds.
What keeps me going is the knowledge that for the time being I am rid of the Leukaemia and the treatment now is to make sure it doesn't come back. So whilst it's tough going I have to try and keep my chin up and keep going, for all that it is difficult on the days when I'm feeling rough and tired.
I have only a few days of this phase of treatment left and will receive my last dose of intra-veinous chemotherapy on Monday, after which I hope to be discharged later in the day so that I can be home for Tom and Sam's 11th birthday which is on Tuesday. I keep reminding the doctors each day to make sure they don't forget that as long as I'm fit enough I want to go home on Monday afternoon!
Beyond that I don't know what the next stage is. I did ask the consultant whether there might be an opportunity for a break to let my body and my senses recover before they attack me again. Unfortunately the answer was probably not much, as the strain of Leukaemia I have is very vigorous and any opportunity my body has to recover also gives the Leukaemia an opportunity to recover and reinfect me, so it doesn't look like a long break will be on the cards.
Either way I'll be grateful of a break at home even if it's only a few days, but have to face the reality that very shortly the next phase of treatment will kick in and once again my body will be punished with more chemotherapy and the like.
Things are improving though and I'm certainly not feeling as rough as I did when I first returned to hospital, when I must have looked like death warmed up. But I'm by no means as chipper as I was through the first phase of treatment when at times I felt better than before the treatment started.
At this time I'm afraid the blog will not be as regular as it was when I started, largely due to the fact that the monotony of the hospital stay gives me little to write about and that on many days I just don't feel up sitting up in bed and writing. I will try and update when I can, particularly as the milestones in my treatment are reached and passed.
All the best everyone and as always, thanks for reading.
I know some of you are concerned about me as I haven't updated the blog for a week so I thought I ought to give you a brief update to let you know I'm still OK.
There is no doubt that this phase of treatment has hit me much harder than the previous phase and it has certainly knocked the stuffing out of me. It has left me feeling tired most of the time, nauseous and sick some of the time, and for the past three weeks I've had almost a constant headache. Consequently most of my days have been spent drifting in and out of sleep due to feeling exhausted and to help pass the days avoiding the pain or sickness I have felt at times.
My energy levels are low anyway as the chemotherapy is designed to inhibit the overall function of my bone marrow as well as attacking the cancerous cells within it. This not only slows down the production of my white cells which have been affected by the Leukaemia but also slows down the red haemaglobin cells which are vital for carrying the oxygen around my body, and the production of platelets which help my blood to clot. As a consequence during this stay in hospital, which has been two and a half weeks so far, I have had three blood transfusions (six units of blood in total), and two transfusions of a unit of platelets. I'm also due to have another unit of platelets before my final lumbar puncture tomorrow.
The stay in hospital is becoming monotonous and tiresome and on many occasions I find the highlight of a morning or afternoon is when the meal trolleys come around and I get something to eat - when I've felt up to eating that is. In between those times I've plugged in my headphones and laid back on my bed listening to music, trying to shut out the sound of what is going on around me which helps me to sleep. At times I've actually slept through the morning or afternoon snack rounds and missed out on a drink of tea, or hot chocolate, and have sometimes found the nurses struggling to wake me from a deep slumber in order to check my blood pressure and temperature when they do the obs rounds.
What keeps me going is the knowledge that for the time being I am rid of the Leukaemia and the treatment now is to make sure it doesn't come back. So whilst it's tough going I have to try and keep my chin up and keep going, for all that it is difficult on the days when I'm feeling rough and tired.
I have only a few days of this phase of treatment left and will receive my last dose of intra-veinous chemotherapy on Monday, after which I hope to be discharged later in the day so that I can be home for Tom and Sam's 11th birthday which is on Tuesday. I keep reminding the doctors each day to make sure they don't forget that as long as I'm fit enough I want to go home on Monday afternoon!
Beyond that I don't know what the next stage is. I did ask the consultant whether there might be an opportunity for a break to let my body and my senses recover before they attack me again. Unfortunately the answer was probably not much, as the strain of Leukaemia I have is very vigorous and any opportunity my body has to recover also gives the Leukaemia an opportunity to recover and reinfect me, so it doesn't look like a long break will be on the cards.
Either way I'll be grateful of a break at home even if it's only a few days, but have to face the reality that very shortly the next phase of treatment will kick in and once again my body will be punished with more chemotherapy and the like.
Things are improving though and I'm certainly not feeling as rough as I did when I first returned to hospital, when I must have looked like death warmed up. But I'm by no means as chipper as I was through the first phase of treatment when at times I felt better than before the treatment started.
At this time I'm afraid the blog will not be as regular as it was when I started, largely due to the fact that the monotony of the hospital stay gives me little to write about and that on many days I just don't feel up sitting up in bed and writing. I will try and update when I can, particularly as the milestones in my treatment are reached and passed.
All the best everyone and as always, thanks for reading.
Subscribe to:
Posts (Atom)